Coronavirus Makes Telehealth a Necessity not just a Convenience

After paying a considerable economic price and human toll, the Chinese people claim to be on track to slowing down the spread of COVID-19 in Wuhan province. That’s encouraging, and may be another reason we don’t need to panic, but it’s also a good time for the rest of the world to wake up and learn quickly from the early mistakes the Chinese made when they got caught off-guard. It’s time to see what was missing in China and prepare better for a Coronavirus that’s now rapidly spreading worldwide scrambling so many aspects of our lives. Beyond starting to test widely based on a smart data-based plan, we also need:
- an efficient and effective way to provide credible and trusted information and advice on what to do and what to avoid (not with loudspeakers broadcasting advice in empty streets.)
- a non-contagious, scalable, and reliable way to triage people to the right level of care (not like this distressed hospital in Wuhan in the early days of the rapid spread.)
- a simple method to deliver care that’s non-contagious, effective, efficient, and scalable (so we don’t need to build hospitals in 6 days.)
Given that a person who contracted the virus can infect between 5–15 people in close proximity, sending people to a healthcare facility unless they need urgent care is a highly risky proposition from a contagion perspective. In addition, too many people who don’t need care will very quickly clog our care healthcare facilities (denying care from other patients who need it more). In an American Hospital Association webinar for hospital administrators, Dr. James Lawler, a professor of Nebraska Medical Center, estimated the disease burden of COVID-19 to be “roughly 10x severe flu season.” Too many patients with mild symptoms would quickly wear-out our healthcare providers, and would effectively create fertile breeding grounds for COVID-19 to propagate and thrive. We need a non-contagious, trusted, effective, and efficient way to solve all of these and provide high quality care to the masses.

To accomplish all of these goals and minimize the risks, we need to quickly create a reliable tiered approach to care and use telehealth and virtual means to accomplish our goals at scale. We will need to:
arm people everywhere with credible bite-size information from doctors available 24/7 at their fingertips on:
- How to prevent contagion
- How to detect potential contagion
- What to do when someone seems to have been infected
- How to care for a person who contracted the virus
We will also need to provide a simple digital triage system that will allow people to input their symptoms in an app or a website and get directed to the right level of care immediately from the convenience and safety of their homes or wherever they might be:
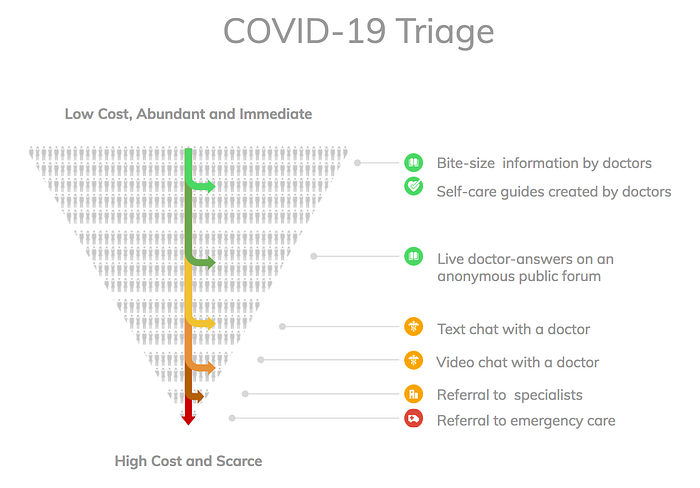
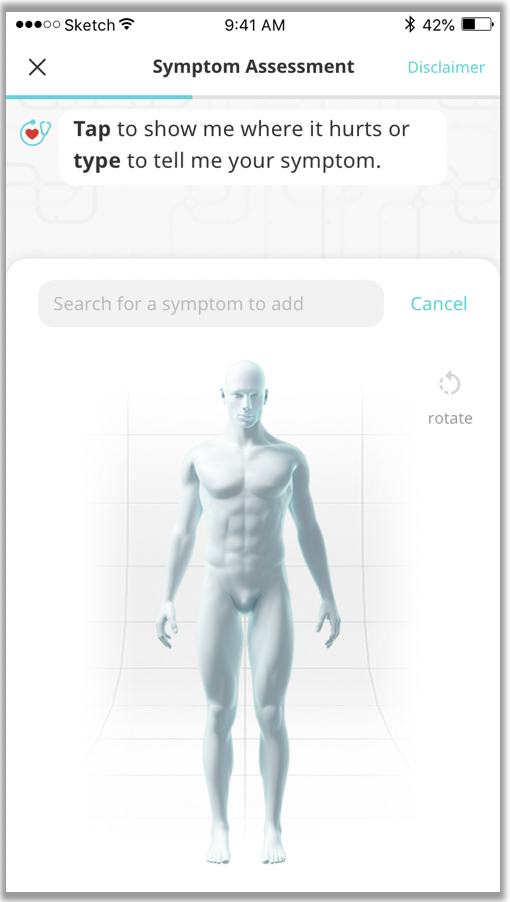
A chat-bot powered by logic can facilitate this kind of initial basic triage (but it’s crucial that it’s trained well, tested thoroughly, and fully validated by doctors for triaging COVID-19.) Also, such chat-bot should only provide recommendations, which can always be overridden by a concerned person who would always be allowed to choose in-person care if she or he feels they must do so. It’s important to give people the confidence that regardless of efficiencies, they remain in control of their destiny and will be taken care of when need be.
For most people experiencing mild symptoms for a short duration of time, and are considered “low risk,” such chat-bot would recommend bite-size information about the how to manage their symptoms at home and and see if it gets better. It can also recommend self-care guides tailored to the person’s characteristics. If the person seems to be at a higher risk, and there are nurses available for telehealth consultations, the chat-bot can direct the cases that are uncertain and not urgent to an available nurse. That nurse can then decide whether to escalate a particular case to a doctor for a telehealth consultation or just arm the patient with a self-care-guide and ask him or her to stay at home and continue to monitoring the progression. If nurses are not available, a person who’s case is above a certain risk threshold (or when he or she chooses to do so) would be directed by the bot to a text or video consultation with a well trained available doctor.
Ideally, the care that doctors provide via text or video consultation would be informed by protocols and procedures for managing people who may have been exposed to or are having symptoms of COVID-19. In addition, leading telehealth providers should continually train their doctors, and provide them with resources and tools to evaluate and take care of all kinds of individuals who will approach them virtually. These need to be regularly updated and made relevant locally based on the spread of the virus and other applicable data and guidance.
When the doctor eventually connects with a patient virtually, the answers that the patient had provided in the chat-bot session would already be available for immediate review by the doctor, which would save both parties precious time. In a world where doctor time is so scarce, every second saved for a doctor can save a life of a person who’s waiting or prevent further contagion by someone who needs to get tested immediatlely. The doctor may then choose to ask additional questions if needed, and make a quick informed assessment, and/or schedule a follow-up telehealth consultation.

If the doctor decides to escalate and send the patient to the testing facility, a clear protocol needs to be in place instructing how to inform both that facility and the authorities of a potential infection. The doctor and/or the telehealth service should then share with the testing facility the data collected from the patient digitally (with the patient’s informed consent.) The same process needs to be applied to a patient who was tested positive for COVID-19, and is in a condition that requires a referral to a specialist and/or a hospital.
Whether the patient tests positive or negative for COVID-19, and based on the patient’s medical state, more than 80% of the time, home quarantine would likely be recommended (unless the community health services designated a special facility for active cases.) In that case, the patient will still need to stay in touch with a healthcare professional (a nurse or a doctor), to monitor their journey to (likely) recovery. The followup consultations, once again, would be done in a much safer and more efficient way using telehealth.
Finally, we will need to also empower patients with easy to understand instructions to help them and their caregivers overcome COVID-19 remotely. To make the recovery process more efficient and effective, care providers should provide their patients with care-guides containing clear guidance on how to manage their condition, and how to avoid infecting others. If the care-guide is digital, it can also provide ongoing reminders, notifications and additional up-to-date information that can help the patient cope and recover faster and the family remain safe and sane. And most importantly, everyone needs to keep in mind that there’s no need to panic — all we need to do is to take a deep breath, prepare and deploy non-contagious means for diagnosis and care— and when we do, almost all of us would and remain healthy and hopefully happy too :)
